Non Surgical Hemorrhoid Treatment Options
March 10, 2026
How to Stop Bleeding Hemorrhoids Safely
March 11, 2026Bleeding after a bowel movement can get your attention fast. So can itching that will not quit, swelling that makes sitting uncomfortable, or the nagging sense that over-the-counter creams are not solving the real problem. For many adults, the next question is simple: is there a treatment that works without surgery, anesthesia, or days away from work?
For the right type of hemorrhoid, the answer is often yes. A hemorrhoid banding procedure is a common office-based treatment designed to relieve internal hemorrhoid symptoms without the disruption of traditional surgery. It is quick, targeted, and usually allows people to return to normal activity the same day.
What is a hemorrhoid banding procedure?
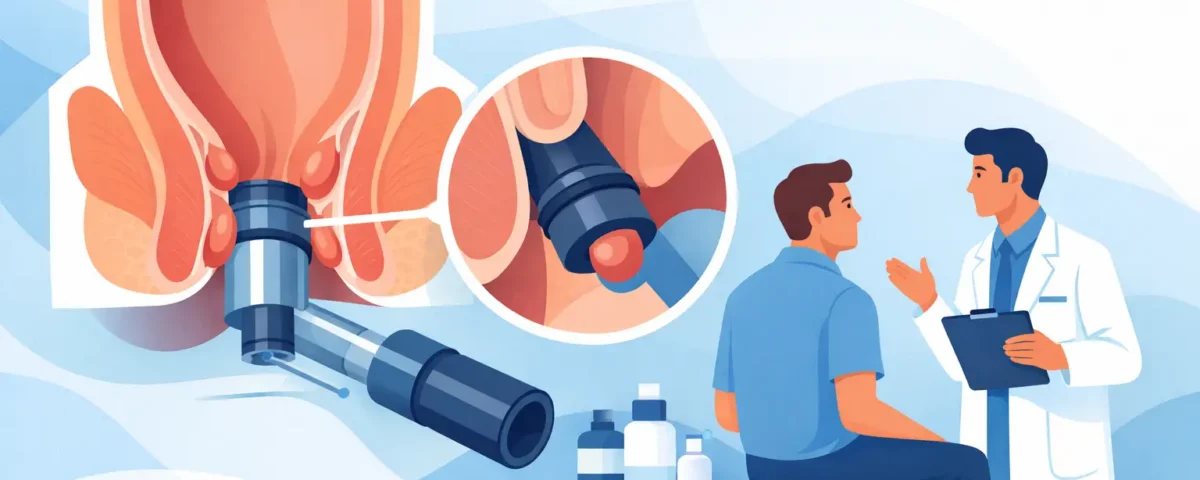
A hemorrhoid banding procedure, also called rubber band ligation, treats internal hemorrhoids by placing a small band around the base of the hemorrhoid inside the rectum. That band cuts off blood flow to the excess tissue. Over time, the treated hemorrhoid shrinks, dries up, and falls away, usually during a bowel movement.
This is not the same as surgery for large external hemorrhoids or more advanced cases that require an operating room. Banding is typically used for internal hemorrhoids that cause bleeding, irritation, prolapse, or a feeling of fullness. Because internal hemorrhoids sit higher in the anal canal where there are fewer pain-sensitive nerves, treatment is often much more tolerable than patients expect.
That distinction matters. Many people assume any hemorrhoid procedure means significant pain and a long recovery. In reality, properly selected patients can often be treated in the office in a matter of minutes.
Who is a good candidate for hemorrhoid banding?
Banding is usually best for internal hemorrhoids, especially when symptoms keep coming back despite diet changes, stool softeners, fiber, hydration, or nonprescription products. If you have repeated bleeding, tissue that protrudes during bowel movements, persistent irritation, or symptoms that interfere with work and daily life, banding may be worth discussing.
It is not ideal for every patient. External hemorrhoids, anal fissures, mixed hemorrhoids, or severe prolapse may call for a different treatment plan. Some people also have bleeding that seems like hemorrhoids but is actually related to another condition. That is one reason a specialist evaluation matters. The goal is not just symptom relief. It is making sure the diagnosis is correct and the treatment matches the problem.
A focused hemorrhoid practice can often identify these differences quickly. That helps patients avoid wasting more time on treatments that were never likely to fix the source of the problem.
What happens during the hemorrhoid banding procedure?
The visit is usually straightforward. After an exam confirms that banding is appropriate, the provider uses a small instrument to gently access the internal hemorrhoid and place a tiny rubber band at its base. The process itself is brief and does not require general anesthesia.
Most patients describe pressure rather than sharp pain. You may feel a sense of fullness or an urge to have a bowel movement for a short time afterward. That sensation is common and usually settles down.
Depending on the number and size of hemorrhoids, more than one treatment may be needed. Not every hemorrhoid should be banded at once. In many cases, staged treatment leads to better comfort and safer healing.
This is one of the key trade-offs patients should understand. Banding is less invasive than surgery, but relief may sometimes happen over a series of visits rather than one major procedure. For many people, that is a worthwhile exchange because it avoids anesthesia, incisions, and a harder recovery.
Does hemorrhoid banding hurt?
This is usually the first concern, and understandably so. The honest answer is that some discomfort is possible, but it is commonly manageable and shorter-lived than people fear.
Because the band is placed on internal hemorrhoid tissue, severe pain is not expected when the procedure is performed correctly on the right patient. Mild pressure, cramping, or a dull ache can happen afterward. Some patients feel almost nothing beyond temporary fullness. Others notice discomfort for a day or two, especially with bowel movements.
Pain that feels intense or steadily worsening is not typical and should be reported. That could mean the band is placed too low or another issue needs attention. A specialized provider will explain what is normal, what is not, and how to handle recovery comfortably.
Recovery after hemorrhoid banding
One reason banding is so appealing is the minimal downtime. Many patients go back to normal routines the same day, though it is smart to keep the rest of the day light if possible. You can usually walk, work, and handle everyday activities without major interruption.
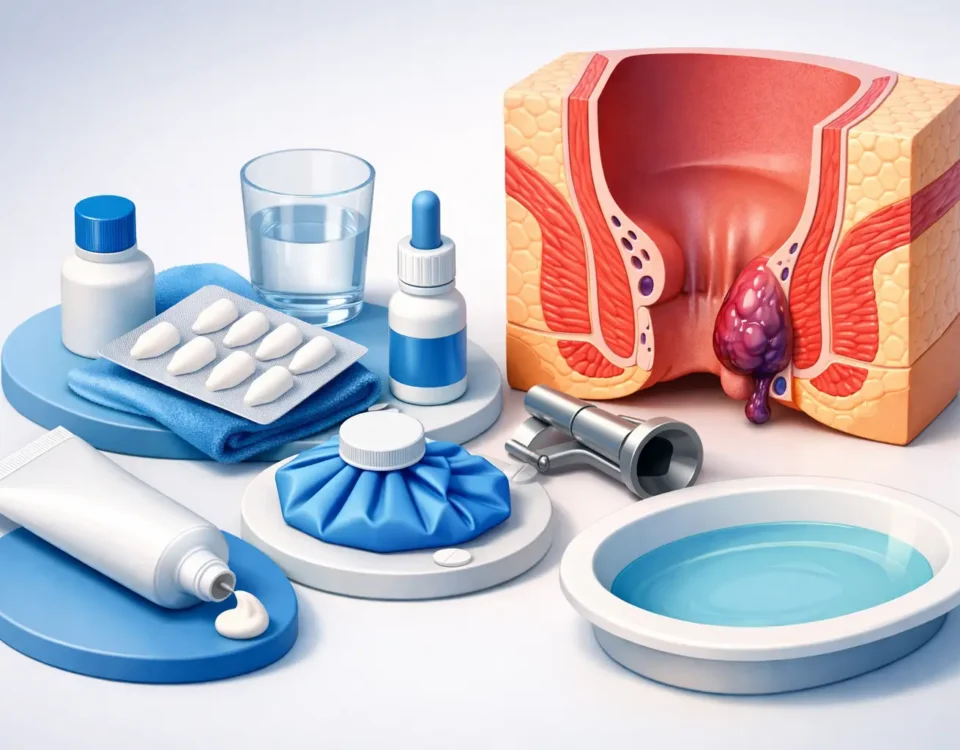
Recovery is less about bed rest and more about protecting the area while healing. That usually means avoiding straining, keeping stools soft, drinking enough water, and following any instructions on fiber or medications. If constipation continues, it can aggravate symptoms and make even a successful treatment feel harder than it should.
A small amount of bleeding can happen when the treated hemorrhoid separates. That is often expected. What should prompt a call is heavy bleeding, fever, severe pain, difficulty urinating, or symptoms that feel clearly outside the normal course explained by your provider.
Most patients start to notice improvement as the treated tissue shrinks and symptoms settle. If there are multiple hemorrhoids or long-standing irritation, full relief may take more than one session.
Benefits of the hemorrhoid banding procedure
The biggest advantage is that it targets the source of internal hemorrhoid symptoms without sending patients down a surgical pathway they may not need. For busy adults, that matters.
Banding is office-based, does not require general anesthesia, and typically involves little downtime. It can be an effective option for bleeding and prolapsing internal hemorrhoids, especially after conservative treatments have failed. It also allows treatment to happen sooner, which is important when symptoms have already started affecting sleep, work, exercise, or confidence in daily life.
There is also a privacy and convenience factor that should not be overlooked. Many people delay care because they are embarrassed or assume treatment will be extreme. A quick, specialized office procedure often feels much more manageable than they imagined.
Limitations and when another treatment may be better
Banding works very well in the right setting, but it is not a cure-all for every anorectal symptom. If the main issue is an anal fissure, a painful thrombosed external hemorrhoid, or advanced prolapse, the treatment plan may look different.
This is where internet advice can lead people astray. The symptom might be bleeding, but the cause is not always the same. Itching and pain can come from several conditions, and treating the wrong problem wastes time and prolongs discomfort.
A good specialist will not force every patient into the same procedure. Sometimes the best next step is custom medication, symptom control first, or a different in-office approach. Sometimes surgery is still appropriate. The point is accurate diagnosis and choosing the least invasive treatment that is likely to work.
When to stop waiting and get evaluated
If you have tried fiber, creams, wipes, sitz baths, and diet changes but symptoms keep returning, that is usually a sign to be seen. Bleeding should not simply be assumed to be hemorrhoids forever. Ongoing swelling, irritation, or tissue prolapse also deserves a proper evaluation.
Waiting often has less to do with the severity of symptoms and more to do with fear. People worry about pain, anesthesia, missing work, or having an awkward conversation. In a focused office setting, those concerns are usually addressed quickly. The evaluation is direct, the treatment options are clear, and many patients find out they are candidates for a non-surgical solution.
For patients who want expert care without the hospital experience, Hemorrhoid Centers of America offers office-based treatment designed around speed, discretion, and relief.
The hardest part for many people is not the procedure. It is deciding they have put up with the symptoms long enough. Once that decision is made, effective treatment is often much simpler than expected.