When Should Hemorrhoids Be Treated?
April 19, 2026If the idea of hemorrhoid treatment makes you picture a hospital, sedation, and days away from work, that is often the first thing to correct. For many patients, a hemorrhoid procedure without anesthesia is not only possible, but also the reason they finally decide to get care. The right office-based treatment can relieve bleeding, swelling, itching, and irritation without the disruption that comes with traditional surgery.
That matters because people usually wait too long. They try creams, wipes, sitz baths, diet changes, and the hope that the problem will settle down on its own. Sometimes symptoms improve for a while. Just as often, the bleeding returns, the swelling flares again, or the discomfort starts interfering with work, exercise, travel, and sleep. At that point, the real question becomes less about whether to seek help and more about what kind of treatment fits real life.
What a hemorrhoid procedure without anesthesia usually means
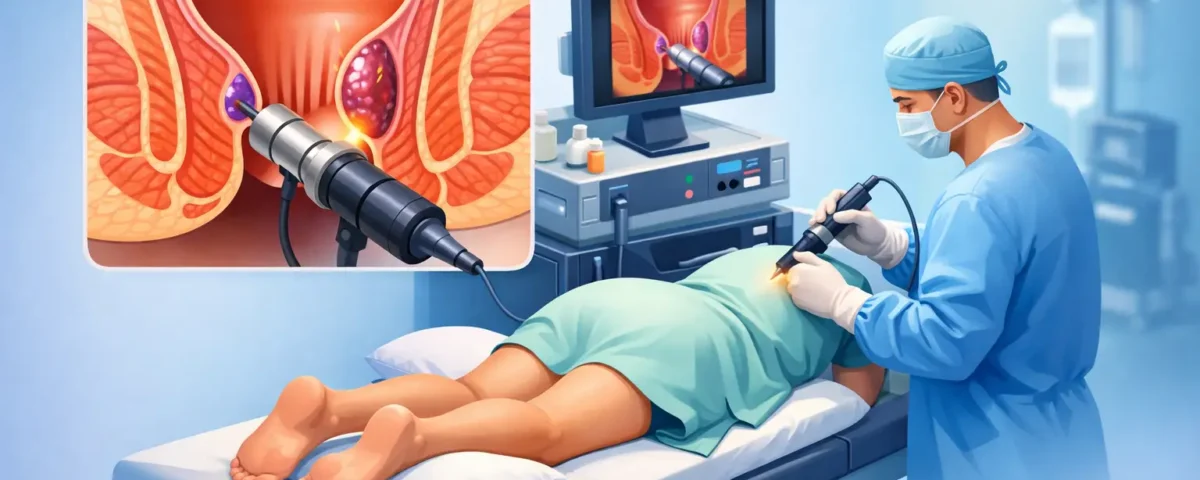
When patients hear the phrase, they often assume it means a painful procedure done with no support at all. That is not what office-based hemorrhoid care is designed to be. In most cases, it refers to a minimally invasive treatment performed in a clinic setting, without general anesthesia or hospital-based sedation.
For internal hemorrhoids, rubber band ligation is one of the most common examples. A board-certified specialist places a small band at the base of the internal hemorrhoid, cutting off its blood supply. The treated tissue then shrinks and resolves over time. Because internal hemorrhoids are located in an area with fewer pain-sensitive nerve endings than external tissue, many patients tolerate this well without anesthesia.
That does not mean every patient feels the exact same thing. Some feel pressure. Some notice a sense of fullness or an urge to have a bowel movement for a short period after treatment. A smaller number feel more discomfort and may need closer follow-up or adjustments in treatment planning. The point is not that the procedure feels like nothing. The point is that it is often manageable, brief, and far less disruptive than people expect.
Why patients look for treatment without anesthesia
The interest is usually practical, not cosmetic. Most adults searching for a hemorrhoid procedure without anesthesia want to avoid the cascade that often comes with surgery – pre-op instructions, fasting, arranging a ride, time off work, and a longer recovery.
They also want privacy and speed. An office visit that leads to diagnosis and treatment can feel much more approachable than entering a hospital system for a condition many people already feel embarrassed to discuss. For working adults, caregivers, and anyone with a packed schedule, avoiding anesthesia often means avoiding a full day built around the procedure.
There is also a medical reason this approach appeals to patients. Anesthesia itself adds another layer of risk, preparation, and monitoring. For the right hemorrhoid type, avoiding it can simplify care substantially.
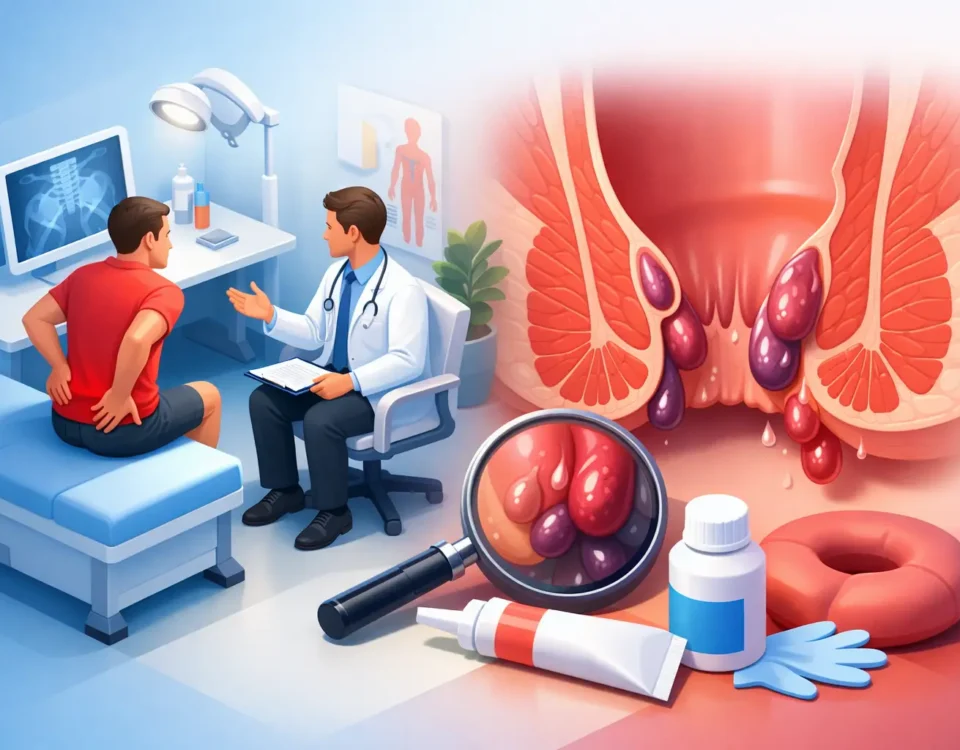
Who is a good candidate
Not every hemorrhoid problem should be treated the same way. That is why evaluation matters. Internal hemorrhoids that cause bleeding, prolapse, irritation, or recurrent flare-ups are often the best fit for office-based banding or similar non-surgical approaches.
Patients with large external hemorrhoids, mixed internal and external disease, thrombosed hemorrhoids, or another anorectal condition may need a different plan. Anal fissures, for example, can cause sharp pain and bleeding but are treated differently from hemorrhoids. Skin tags, abscesses, fistulas, and more serious colorectal conditions can also mimic hemorrhoid symptoms.
This is one reason specialized care matters. The best treatment is not the least invasive option at all costs. It is the least invasive option that is actually appropriate and likely to work.
What the procedure feels like
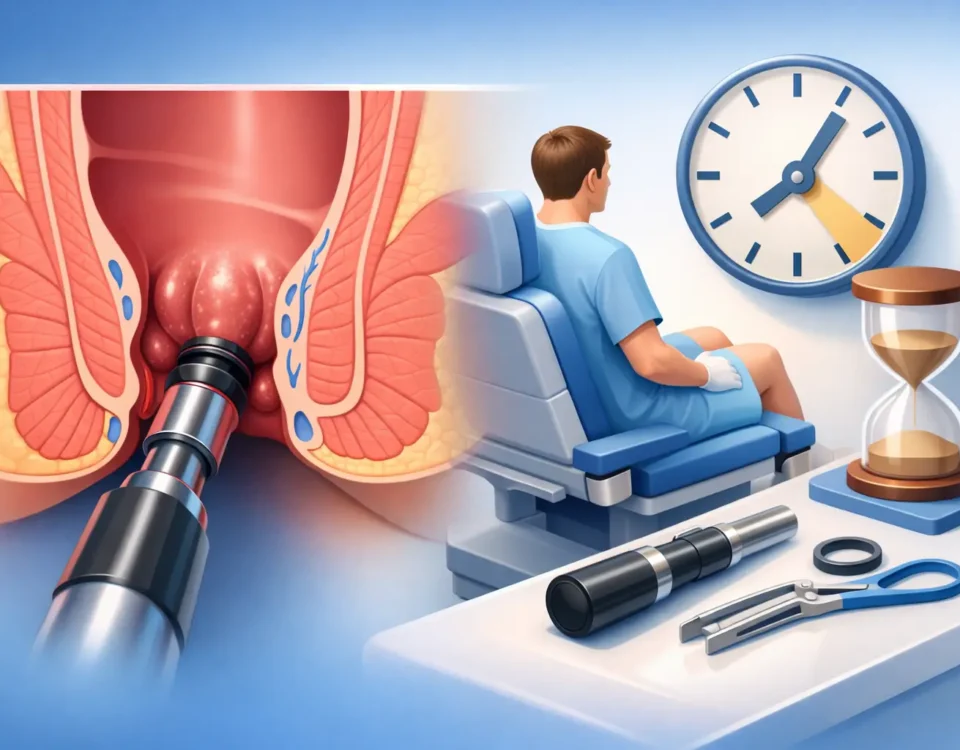
This is usually the part patients care about most, and understandably so. In an office-based hemorrhoid procedure without anesthesia, treatment is generally quick. The actual procedure may take only a few minutes.
During internal hemorrhoid banding, patients often describe pressure rather than sharp pain. Afterward, it is common to feel mild cramping, fullness, or awareness in the rectal area for a short time. Most patients are able to walk out of the office and resume normal light activity the same day.
There is still some variability. If a hemorrhoid is more advanced, if multiple areas require treatment over time, or if a patient has heightened sensitivity, recovery may feel less straightforward. Good treatment planning takes that into account. Specialists often stage care instead of trying to do too much at once, which can make the experience easier to tolerate and improve outcomes.
The real advantage is not just comfort
Avoiding anesthesia is appealing, but the larger benefit is efficiency. Office-based hemorrhoid care can remove a major barrier to treatment. When the process is simpler, patients are more likely to stop delaying care and deal with the problem before symptoms worsen.
That can have a real quality-of-life effect. Ongoing bleeding creates stress. Recurrent swelling changes how people sit, exercise, travel, and even dress. Persistent itching or irritation can become a daily distraction. A fast, focused treatment plan helps patients get relief without putting the rest of life on hold.
For many people, that balance is the whole point. They are not looking for a dramatic surgical solution. They want effective care from a specialist who treats this problem routinely, in a setting that does not feel overwhelming.
Recovery after a hemorrhoid procedure without anesthesia
Recovery is usually one of the strongest reasons patients choose this route. Most office-based treatments involve little downtime. Many people return to desk work, normal errands, and routine daily activity the same day or the next day, depending on how they feel.
That said, easy recovery does not mean no aftercare. Patients are still typically advised to stay hydrated, avoid straining, support bowel regularity, and follow any medication instructions carefully. If constipation is part of the original problem, that issue has to be addressed or symptoms may recur.
Some patients need more than one treatment session. That is not a sign of failure. Hemorrhoids can vary in size, number, and severity, and a staged plan is often the most effective and comfortable approach.
Why over-the-counter treatment is not the same thing
A common pattern is trying nonprescription products for months before seeking medical care. Creams and suppositories can temporarily reduce irritation, but they usually do not eliminate the underlying hemorrhoid tissue that keeps causing trouble.
That is where procedure-based care becomes different. It is not just symptom management. It is an attempt to treat the source of recurrent bleeding or prolapse directly.
There is a trade-off here. Conservative care is easy to start and useful for mild flare-ups. But if symptoms keep returning, continuing the same home remedies can drag out the problem and prolong discomfort.
When to stop waiting
Bleeding with bowel movements, tissue that protrudes, ongoing itching, recurrent swelling, and discomfort that keeps coming back are all reasons to get evaluated. So is any uncertainty about what is causing your symptoms.
Patients sometimes assume all rectal bleeding is from hemorrhoids. That is a risky assumption. While hemorrhoids are common, bleeding should be assessed properly, especially if symptoms are new, changing, or paired with other bowel changes.
A focused exam can usually clarify what is happening quickly. For the right patient, treatment may be far more straightforward than expected.
Choosing the right specialist
Experience matters in this area because accuracy matters first. You want a provider who treats hemorrhoids and fissures routinely, understands when non-surgical care is appropriate, and does not push patients toward unnecessary surgery.
You also want realistic counseling. Good care is not about promising that every case is painless or that every symptom disappears overnight. It is about matching the treatment to the diagnosis, setting clear expectations, and helping patients get meaningful relief with as little disruption as possible.
That is why specialized centers such as Hemorrhoid Centers of America focus on office-based treatment pathways designed around speed, convenience, and effective non-surgical care.
If you have been putting this off because you are worried about pain, anesthesia, or losing time from your routine, it may help to know that treatment is often much simpler than people imagine. The hardest part is usually deciding to get it checked.