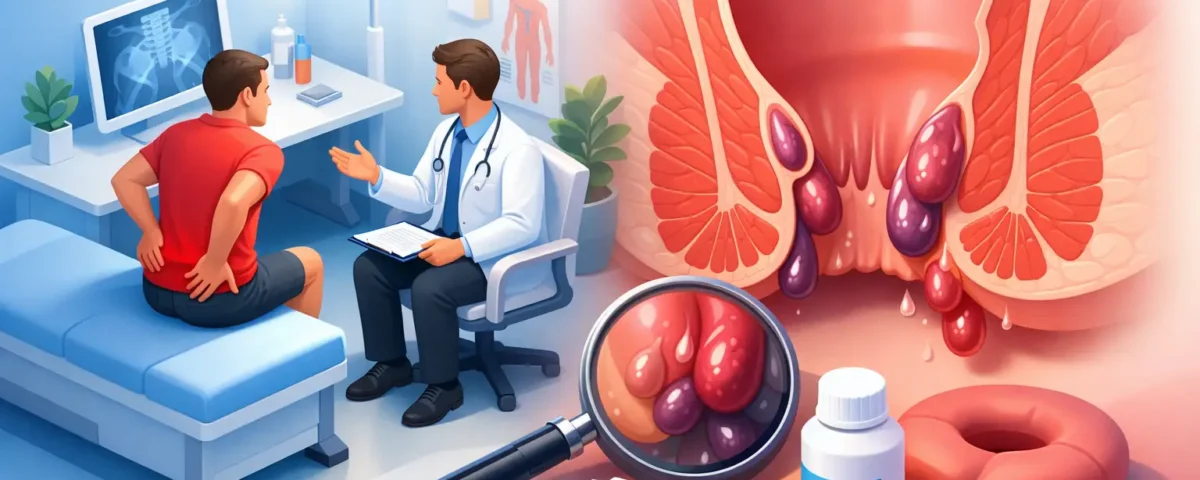
Top Treatments for Bleeding Hemorrhoids
April 13, 2026
How Long Hemorrhoid Banding Takes
April 17, 2026You notice blood on the toilet paper, some itching that will not let up, or a painful lump that suddenly makes sitting uncomfortable. That is usually the point when people start asking when to see a doctor for hemorrhoids. The short answer is this: if symptoms are persistent, painful, bleeding, or getting worse, it is time to stop guessing and get evaluated.
Many hemorrhoids do improve with basic home care. But not every case should be handled with creams, wipes, and wishful thinking. Hemorrhoids can range from mild irritation to significant swelling, ongoing bleeding, and pain that interferes with work, sleep, exercise, or bowel movements. In some cases, what seems like a hemorrhoid may actually be a different condition that needs medical attention.
When to see a doctor for hemorrhoids
A good rule is to seek care if symptoms last more than about a week despite home treatment, or sooner if you have heavy bleeding, severe pain, or a lump that appears suddenly and feels very tender. Hemorrhoids are common, but that does not mean you should have to live with them.
You should also schedule an appointment if bowel movements have become something you dread. Ongoing pain, burning, itching, or a feeling of pressure in the rectal area are signs that the problem is no longer minor. The same is true if symptoms keep returning. Repeated flare-ups often mean the underlying issue has not been resolved.
For many patients, the real reason they delay care is not uncertainty about symptoms. It is embarrassment, fear of surgery, or concern about missing work. That hesitation is understandable, but it often keeps people uncomfortable longer than necessary. A specialist can usually tell fairly quickly what is going on and whether non-surgical treatment is appropriate.
Symptoms that should not be ignored
Rectal bleeding is the symptom people most often associate with hemorrhoids, but it should never be brushed off automatically. Small amounts of bright red blood can happen with hemorrhoids, especially after straining, but any bleeding from the rectum deserves proper evaluation. Bleeding can also come from anal fissures, inflammation, polyps, or other gastrointestinal conditions.
Pain is another sign worth taking seriously. Internal hemorrhoids do not always hurt, but external hemorrhoids can become very painful, especially if a clot forms inside them. This is called a thrombosed external hemorrhoid. It may cause sudden swelling and a firm, tender lump near the anus. In that situation, waiting it out can be miserable, and prompt treatment may provide faster relief.
Itching and irritation are sometimes dismissed as minor, but they matter too if they are persistent. Constant itching can mean inflamed hemorrhoidal tissue, excess moisture, skin irritation, or another anorectal problem. If over-the-counter products are not helping, continued self-treatment can actually make the skin more irritated.
Prolapse is another reason to be evaluated. This happens when internal hemorrhoids bulge outside the anus, especially during bowel movements. At first, the tissue may go back in on its own. Later, it may need to be pushed back manually, or it may stay outside. Once prolapse becomes frequent, symptoms often become harder to control at home.
When bleeding means you should be seen sooner
Not all bleeding carries the same level of urgency. A streak of bright red blood once or twice may not be an emergency, but it still should be discussed with a doctor if it recurs. If bleeding is happening regularly, if it is more than a small amount, or if you feel weak, dizzy, or short of breath, you need prompt medical attention.
The same goes for changes in bowel habits along with bleeding. If you have constipation, diarrhea, narrower stools, unexplained weight loss, abdominal pain, or fatigue, it is important not to assume hemorrhoids are the only cause. Hemorrhoids are common, but they should not become a catch-all explanation for every rectal symptom.
Age and personal history matter too. If you are older, have a family history of colorectal disease, or have never had bleeding evaluated before, a proper exam becomes even more important.
Severe pain usually means do not wait
Mild soreness may improve with warm baths, stool softening, hydration, and reduced straining. Severe pain is different. If sitting, walking, or having a bowel movement becomes sharply painful, it is time to be examined.
Pain that starts suddenly often points to a thrombosed external hemorrhoid or an anal fissure. Those conditions can feel similar to patients, but treatment may differ. That is one reason a specialist evaluation matters. The right diagnosis leads to faster relief, while the wrong self-treatment can prolong the problem.
If you see swelling that is increasing instead of settling down, that is another sign to move quickly. The longer significant inflammation continues, the more disruptive symptoms tend to become.
What if home treatment is not working?
Most people try something at home first, and that is reasonable. Increasing fiber, drinking more water, avoiding straining, using sitz baths, and trying short-term over-the-counter products can help mild symptoms. But home care has limits.
If symptoms are unchanged after a week, or if they improve briefly and keep coming back, that is a sign you may need more than symptom management. It is especially true if the issue is affecting your routine. Missing workouts, avoiding travel, sitting gingerly through meetings, or planning your day around discomfort is not a minor problem.
There is also a trade-off with repeated self-treatment. The longer you rely on temporary remedies, the longer inflamed tissue may continue to flare. Some topical products are not meant for extended use, and overuse can irritate sensitive skin.
What to expect at a hemorrhoid evaluation
A lot of anxiety comes from not knowing what the visit will be like. In reality, a hemorrhoid evaluation is usually straightforward and focused. The goal is to confirm whether you have internal hemorrhoids, external hemorrhoids, an anal fissure, or another condition causing similar symptoms.
Your provider will ask about bleeding, pain, bowel habits, and how long symptoms have been going on. A physical exam may be all that is needed to identify external hemorrhoids or fissures. Internal hemorrhoids may require a brief in-office exam to see the swollen tissue more clearly.
The value of seeing a specialist is that the conversation moves quickly from diagnosis to treatment options. If your symptoms are due to internal hemorrhoids, non-surgical procedures may be available that are performed in the office without the kind of downtime people often fear. That can be a major relief for patients who have delayed care because they assumed the only next step was surgery.
At Hemorrhoid Centers of America, treatment is centered on non-surgical options designed to relieve bleeding, pain, swelling, and itching efficiently, often with minimal disruption to the day.
Why earlier treatment can make life easier
People often wait until symptoms become unbearable. The problem with that approach is simple: the longer hemorrhoids remain irritated, the more likely they are to interfere with daily life. Earlier care can mean treating the problem before bleeding becomes frequent, before prolapse worsens, or before pain becomes severe.
That does not mean every hemorrhoid needs a procedure right away. Some cases respond well to conservative care. But a proper evaluation helps determine where you fall on that spectrum. It replaces guesswork with a clear plan.
For working adults, caregivers, and anyone with a busy schedule, that matters. Quick diagnosis and office-based treatment can be very different from the hospital-based experience many people imagine.
The bottom line on when to see a doctor for hemorrhoids
If you have persistent bleeding, significant pain, recurring symptoms, prolapse, or a sudden tender lump, do not keep waiting for it to resolve on its own. And if you are simply not sure whether it is really a hemorrhoid, that is reason enough to be evaluated.
You do not need to be in crisis to seek help. Often, the best time to act is when symptoms first start affecting your comfort, confidence, or routine. Getting the right diagnosis early can spare you weeks or months of avoidable discomfort and get you back to normal faster.