When to See a Doctor for Hemorrhoids
April 15, 2026
When Should Hemorrhoids Be Treated?
April 19, 2026If you are dealing with bleeding, itching, or swelling and trying to fit treatment into a normal workweek, one of the first questions you probably have is how long hemorrhoid banding takes. That question matters because most people are not just looking for relief – they want a treatment that does not turn into a hospital-style event with anesthesia, a long recovery, or days away from work.
For many patients, hemorrhoid banding is surprisingly quick. The actual procedure is often done in minutes, and the full office visit is usually much shorter than people expect. That said, the exact timing depends on your symptoms, how many hemorrhoids are being treated, and whether your provider confirms that banding is the right option for you.
How long hemorrhoid banding takes at the appointment
The banding portion itself is typically very brief. In many cases, placing a band on an internal hemorrhoid takes only a few minutes. If more than one hemorrhoid needs attention over time, treatment may be staged across more than one visit rather than handled all at once.
The office appointment is usually longer than the procedure itself because it includes evaluation, examination, and discussion. A provider needs to confirm the source of your symptoms first. Bleeding, irritation, and rectal discomfort are common with hemorrhoids, but they are not exclusive to hemorrhoids. That is why a proper diagnosis comes before treatment.
For most patients, the full visit may take roughly 30 minutes to an hour, depending on the clinic workflow and the complexity of the case. Some people come in expecting a major procedure and are relieved to find that hemorrhoid banding is handled in an office setting without the long process associated with surgery.
What happens before the banding procedure
Before treatment starts, your provider will review your symptoms, medical history, and any past attempts at relief. That may include over-the-counter creams, fiber supplements, sitz baths, or previous procedures. This part is important because not every hemorrhoid needs the same approach.
Next comes the exam. Internal hemorrhoids are often the ones treated with rubber band ligation, also called hemorrhoid banding. External hemorrhoids are different, and a fissure or another anorectal condition can cause similar symptoms. A focused exam helps identify what is actually causing the problem and whether banding is likely to help.
If you are a candidate, your provider can often move directly into treatment. That efficiency is one reason patients seek out a specialized hemorrhoid practice instead of waiting for a hospital-based surgical pathway.
Does hemorrhoid banding require prep?
Usually, prep is minimal compared with a surgical procedure. Most patients do not need anesthesia, bowel prep, or a full day blocked off for recovery. You may be given simple instructions about eating, medications, or what to expect afterward, but this is generally a straightforward office visit.
That simplicity is a major reason people choose banding when appropriate. It is designed to treat internal hemorrhoids without the disruption that comes with traditional surgery.
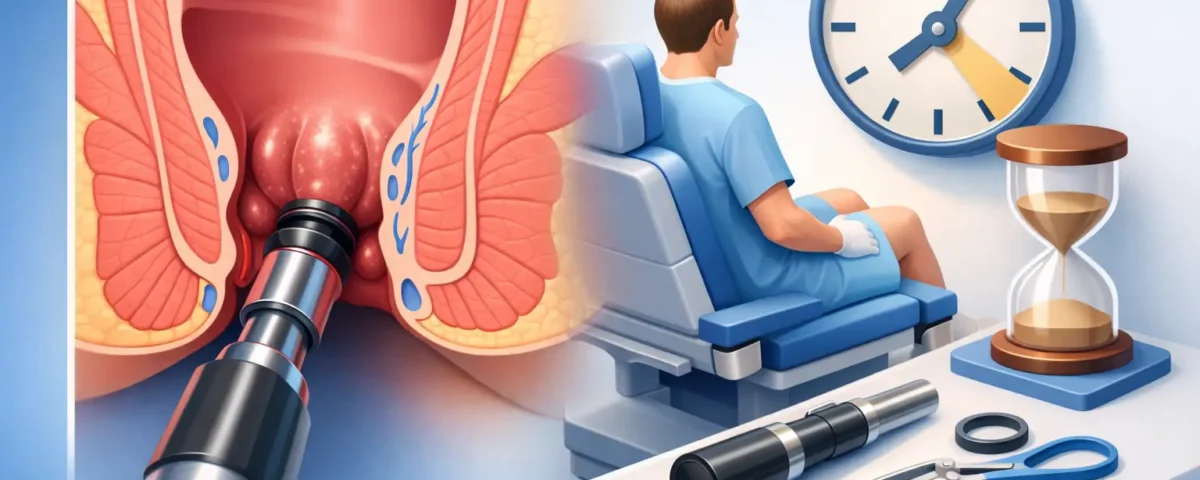
How the procedure works
During hemorrhoid banding, a small rubber band is placed around the base of the internal hemorrhoid. The goal is to cut off its blood supply so the treated tissue shrinks and eventually falls away. Because internal hemorrhoids are located in an area with fewer pain-sensitive nerve endings, the procedure is often more tolerable than patients fear.
Most people feel pressure or a sense of fullness rather than sharp pain during the band placement. If significant pain occurs, that can suggest the band is not positioned correctly and needs adjustment. In a specialized setting, that distinction is well understood.
The procedure is quick, but precision matters. The value is not just speed. It is speed combined with correct diagnosis, proper technique, and a treatment plan built around your symptoms.
How long hemorrhoid banding takes to recover from
Recovery is another area where patients want a clear answer, and the honest answer is that recovery is usually short, but not identical for everyone. Many people return to normal daily activity the same day. Others prefer to take it easy for the rest of the afternoon, especially if they feel mild pressure or cramping.
This is very different from surgical hemorrhoid treatment, which can involve anesthesia, more pain, and a longer recovery period. With banding, the goal is effective relief with minimal downtime.
You may notice mild discomfort, pressure, or the urge to have a bowel movement for a short time after the procedure. Some patients have very little interruption at all. Others need a day or two before everything feels fully settled. The variation usually comes down to your anatomy, the severity of the hemorrhoids, and how your body responds.
When do symptoms start improving?
Some symptoms improve quickly, especially if the treated hemorrhoid was a major source of bleeding or irritation. In other cases, relief is more gradual. The banded tissue generally shrinks over several days, and the hemorrhoid may fall off within about a week.
That does not always mean every symptom disappears overnight. If you have multiple internal hemorrhoids, your provider may recommend more than one treatment session to get the best result while keeping discomfort and risk low.
Why treatment time can vary
When patients ask how long hemorrhoid banding takes, they are often really asking two questions at once: how long will I be in the office, and how long until this problem is behind me? Those answers are related, but they are not exactly the same.
A single office visit can be short, yet the overall treatment plan may unfold over multiple appointments if several hemorrhoids need to be addressed. That is not a sign the treatment is failing. In many cases, it is the safer and more effective way to manage the condition.
Timing can also vary if your symptoms are caused by more than one issue. For example, someone may have internal hemorrhoids along with an anal fissure, constipation, or irritation from straining. In that situation, banding may be one part of treatment rather than the whole plan.
What to expect after you leave the office
Most patients are able to walk out of the appointment and return to routine activity with few restrictions. You may be told to avoid heavy straining and to keep bowel movements soft with hydration, fiber, or other supportive measures. Those aftercare steps matter because they reduce pressure on the treated area and support healing.
A small amount of bleeding can happen when the banded tissue separates. Mild soreness can happen too. Severe pain, heavy bleeding, fever, or trouble urinating are not typical and should be reported promptly.
This is where specialized follow-up matters. A focused hemorrhoid practice can tell you what is normal, what is temporary, and when something needs attention.
Is hemorrhoid banding worth it if your schedule is tight?
For many working adults, parents, and older patients who have already spent too long managing symptoms at home, the answer is yes. The appeal is not just that the procedure is fast. It is that the process is efficient from start to finish: office-based care, no anesthesia in most cases, and little interruption to normal life.
That said, banding is not the right solution for every person with hemorrhoid symptoms. The best results come when the diagnosis is accurate and the treatment matches the type of hemorrhoid involved. A quick procedure still needs thoughtful medical judgment behind it.
If you have been delaying care because you assume treatment will be painful, invasive, or time-consuming, this is where a specialist evaluation can change the picture. At Hemorrhoid Centers of America, the focus is on non-surgical treatment that fits real life while still delivering meaningful symptom relief.
The most useful next step is not guessing how long you can keep living with the symptoms. It is finding out whether a short office procedure could finally give you a clear path back to normal.