Office Based Hemorrhoid Treatment Explained
March 20, 2026
Same Day Hemorrhoid Treatment Options
March 22, 2026If you are searching for hemorrhoid treatment no anesthesia, you are probably not looking for a long lecture. You want to know whether there is a real option that relieves pain, bleeding, swelling, or itching without a hospital visit, sedation, or a difficult recovery. In many cases, the answer is yes.
For the right patient, hemorrhoids can often be treated in an office setting with minimally invasive care that does not require anesthesia. That matters because fear of surgery keeps a lot of people waiting too long. By the time they come in, they have already tried creams, wipes, fiber, and home remedies, yet the symptoms keep coming back.
When hemorrhoid treatment with no anesthesia makes sense
Not every hemorrhoid needs a procedure, and not every patient needs the same plan. Mild symptoms may improve with changes in bowel habits, hydration, fiber intake, and targeted medication. But when symptoms are persistent, recurring, or disruptive, office-based treatment often becomes the more effective option.
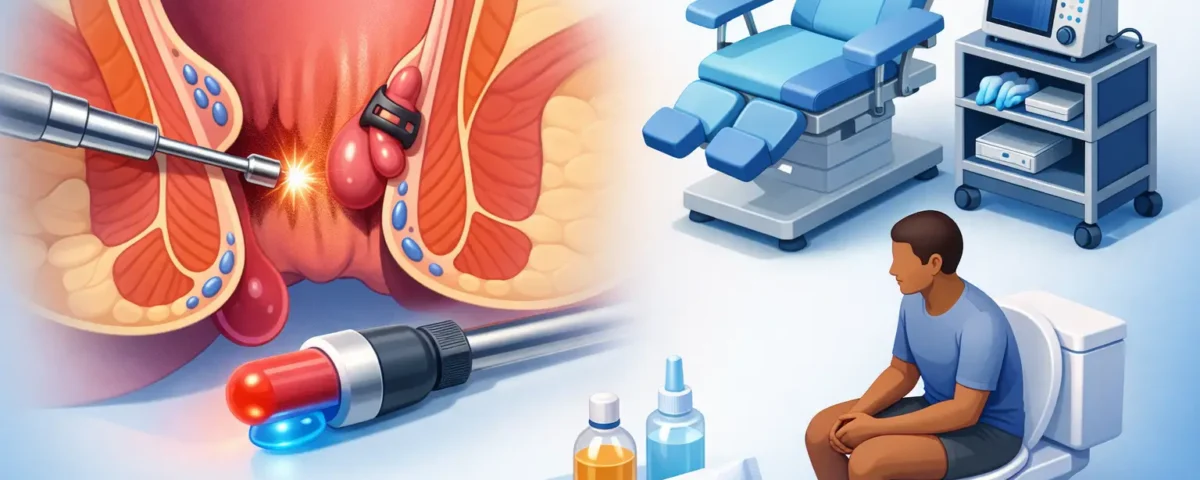
This is especially true for internal hemorrhoids that bleed, prolapse, or create ongoing irritation. These hemorrhoids are often good candidates for hemorrhoid banding, a non-surgical treatment performed without traditional anesthesia. The goal is straightforward – treat the source of the problem directly, avoid unnecessary surgery, and get you back to normal life quickly.
External hemorrhoids are a little different. If the main issue is a painful external clot or significant swelling, the treatment path may not be the same as it is for internal hemorrhoids. That is one reason a proper exam matters. People often assume they have hemorrhoids when they may actually have an anal fissure, skin tags, irritation, or another anorectal condition that needs a different approach.
What hemorrhoid treatment no anesthesia usually involves
The most common office-based procedural option is hemorrhoid banding. During this treatment, a provider places a small band around the base of an internal hemorrhoid. This cuts off its blood supply so the tissue shrinks and resolves over time.
For many patients, the appeal is obvious. There is no operating room, no general anesthesia, and no hospital-style recovery. The procedure is typically brief, and most people are able to return to normal daily activity the same day.
That does not mean the experience is identical for everyone. Some patients feel pressure or a sense of fullness afterward. Others have very little discomfort. Symptom severity, hemorrhoid size, and the exact area being treated can all affect how you feel after the procedure. A specialized provider will explain what is normal and what would be considered unusual.
Why many patients prefer to avoid anesthesia
For adults balancing work, family responsibilities, and everyday obligations, anesthesia is not a small detail. It can mean extra preparation, transportation planning, more time off, and a longer recovery window. Some patients also have health concerns that make them want to avoid sedation when possible.
That is why no-anesthesia hemorrhoid treatment appeals to so many people. It removes one of the biggest psychological barriers to care. Instead of picturing surgery, patients can focus on an office visit designed to treat the problem efficiently.
There is also a practical benefit. Treatments that avoid anesthesia often allow for faster recovery and less disruption to your schedule. If your symptoms are affecting your workday, sleep, exercise routine, or comfort during bowel movements, that kind of efficiency matters.
What an office visit typically looks like
The first step is evaluation. A board-certified specialist reviews your symptoms, asks how long they have been happening, and performs an exam to confirm what is causing the problem. This step is important because rectal bleeding, pain, and irritation are not exclusive to hemorrhoids.
Once the diagnosis is clear, the provider can recommend the right plan. Sometimes that means medical management first. Sometimes it means office-based banding. In other cases, a staged approach works best, especially if there are multiple hemorrhoids or a combination of hemorrhoids and fissure symptoms.
The procedure itself is usually quick. Patients often expect something much more dramatic than what actually happens. For suitable internal hemorrhoids, treatment can be completed in the office without the steps involved in surgical care.
Afterward, you may be given instructions about bowel habits, hydration, activity, and what to expect over the next several days. Good follow-up matters because long-term relief is not only about treating the current hemorrhoid. It is also about reducing the factors that contributed to it in the first place, such as constipation, straining, prolonged sitting, or repeated irritation.
Is no-anesthesia hemorrhoid treatment effective?
For properly selected patients, yes. Office-based banding is a well-established treatment for internal hemorrhoids and can be very effective for bleeding, prolapse, and recurrent symptoms that have not responded to conservative care.
The key phrase is properly selected. This is not a one-size-fits-all solution. A patient with severe external disease, a large thrombosed hemorrhoid, or another anorectal condition may need a different treatment plan. That is why specialized evaluation matters more than trying to guess the right option from symptoms alone.
Experience also matters. A provider who focuses specifically on hemorrhoid and fissure care is better positioned to recognize which symptoms are likely to improve with office treatment and which need a different path. That focused approach can help patients avoid both undertreatment and unnecessary surgery.
What recovery is really like
Most patients want the honest version, not the overly polished one. The honest version is that recovery after office-based hemorrhoid treatment is usually manageable, but it is not identical for everyone.
Many people return to normal routine the same day. Some feel mild pressure, temporary urgency, or irritation. Small amounts of bleeding can occur depending on the stage of healing. Bowel movements may feel different for a short time, especially if you were already inflamed before treatment.
What usually makes recovery easier is following instructions closely. Staying hydrated, using fiber appropriately, avoiding straining, and keeping stools soft can make a significant difference. If your symptoms included chronic constipation or long periods on the toilet, changing those habits is part of treatment, not an optional extra.
When to stop waiting
A lot of patients delay care because they hope the problem will settle down on its own. Sometimes it does. Often it improves, then flares again. Bleeding returns. Swelling returns. The itching keeps interrupting your day. You start planning around discomfort.
That is usually the point where office-based treatment becomes worth serious consideration. If you have already tried over-the-counter products and your symptoms keep coming back, getting examined is not overreacting. It is the practical next step.
You should also stop waiting if you are having recurrent rectal bleeding, tissue prolapse, ongoing pain, or symptoms that are affecting work, exercise, or sleep. Even if the final diagnosis is not hemorrhoids, it is better to know what you are dealing with and treat it correctly.
Choosing a provider for hemorrhoid treatment no anesthesia
Because this is such a specific area of care, specialization matters. Patients generally do better when they are evaluated by providers who treat hemorrhoids and fissures routinely, rather than as a small part of a much broader practice.
Ask direct questions. Is the treatment performed in the office? Is anesthesia typically required? What kind of recovery should you expect? Are they evaluating for fissures and other causes of symptoms as well? Clear answers are a good sign that the practice is experienced and focused.
At Hemorrhoid Centers of America, that focus is central to the patient experience. The goal is not to funnel every patient toward surgery. It is to diagnose the problem accurately, recommend the least disruptive effective treatment, and help patients get relief without unnecessary delays.
If embarrassment has kept you from making an appointment, you are not alone. But this is a very common medical issue, and it is one that often has a faster, easier treatment path than people expect. Relief does not always require surgery, and it does not always require anesthesia. For many patients, the hardest part is simply deciding they are done living with it.