Does Hemorrhoid Banding Hurt?
March 19, 2026
Hemorrhoid Treatment No Anesthesia Options
March 21, 2026If you’re timing bathroom trips around meetings, packing extra wipes in your work bag, or worrying about bleeding every time you sit down, the problem has already started affecting more than your comfort. Office based hemorrhoid treatment is designed for exactly this kind of situation – when symptoms are real, disruptive, and not improving with creams, fiber, or waiting it out.
For many adults, the biggest barrier is not the symptoms themselves. It’s the assumption that treatment means hospital surgery, anesthesia, and days away from work. In many cases, that is not true. Hemorrhoids can often be treated in a medical office with minimally invasive procedures that target the source of bleeding, swelling, itching, and irritation without the disruption of traditional surgery.
What office based hemorrhoid treatment actually means
Office based hemorrhoid treatment refers to procedures and care delivered in a clinic setting rather than a hospital or surgery center. The goal is straightforward: relieve symptoms efficiently, avoid unnecessary surgery when possible, and get patients back to normal activity quickly.
That matters because hemorrhoids are not all the same. Some are primarily internal and bleed. Others swell, prolapse, or cause ongoing irritation. Some patients also have an anal fissure, which can create sharp pain that feels very different from hemorrhoid discomfort. A focused evaluation is what separates effective treatment from another round of guesswork.
In an office setting, the provider can identify what is actually causing the symptoms and recommend a treatment plan based on severity, location, and how long the problem has been going on. For many patients, that plan includes hemorrhoid banding, medication, or a combination of both.
Why patients choose office based hemorrhoid treatment
Most people do not seek care the first week symptoms appear. They try over-the-counter products, adjust their diet, sit on a cushion, and hope the problem settles down. Sometimes mild symptoms improve. But when bleeding keeps happening, swelling returns, or discomfort starts interfering with work, exercise, travel, or sleep, temporary measures stop feeling like a solution.
This is where office based care becomes appealing. It is private, fast, and usually much less disruptive than patients expect. You are seen by a medical provider who treats this condition regularly, the evaluation is focused, and treatment is often performed without general anesthesia. For working adults and anyone with a busy schedule, that difference matters.
There is also a psychological benefit. Hemorrhoids are common, but patients often delay care because they feel embarrassed. A specialized office that treats anorectal conditions every day can make the process feel much more routine and manageable.
The most common office based hemorrhoid treatment options
The right treatment depends on the type and grade of hemorrhoid, your symptoms, and whether there are other issues contributing to pain or bleeding.
Hemorrhoid banding
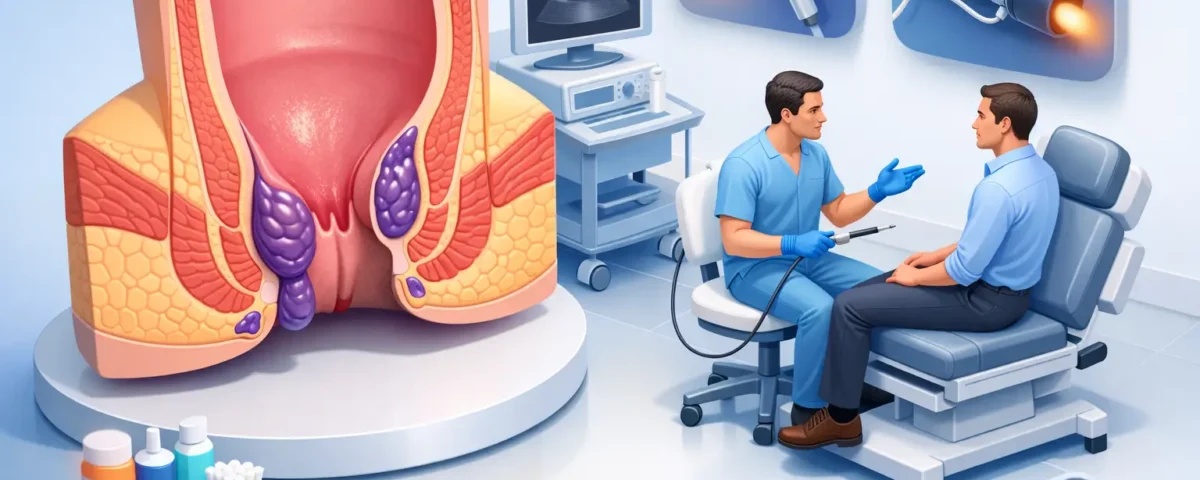
Rubber band ligation, often called hemorrhoid banding, is one of the most effective office-based treatments for internal hemorrhoids. During the procedure, a small band is placed around the base of the hemorrhoid to cut off its blood supply. The tissue then shrinks and resolves over time.
For the right patient, banding can be a strong option because it treats the hemorrhoid directly without the recovery burden associated with surgery. It is commonly used for internal hemorrhoids that bleed, prolapse, or recur despite conservative care.
Patients often ask whether banding is painful. The honest answer is that most people feel pressure or an urge to have a bowel movement rather than sharp pain, because internal hemorrhoids are located in an area with fewer pain-sensitive nerves. Technique matters, which is one reason specialized care is so valuable.
Medication-based treatment
Not every patient needs a procedure on day one. Some benefit from custom medication protocols, especially if inflammation, irritation, or an anal fissure is part of the problem. Targeted medication may help reduce pain, swelling, spasm, and discomfort while supporting healing.
This is one of the trade-offs that matters. A procedure may offer more definitive relief for certain internal hemorrhoids, while medication may be more appropriate for fissures, external irritation, or mixed symptoms. Good care is not about forcing every patient into the same treatment. It is about matching treatment to the actual diagnosis.
When surgery may still be necessary
Office treatment is highly effective for many patients, but not every case belongs in a non-surgical pathway. Large external hemorrhoids, advanced prolapse, thrombosed hemorrhoids, or persistent symptoms despite prior treatment may require a different approach.
That does not mean you should assume surgery first. It means you need an accurate exam. Many patients who fear surgery turn out to be good candidates for office-based care. Others need to understand when a more involved intervention will produce the best long-term result.
What to expect during the visit
The first visit usually starts with a discussion of symptoms – bleeding, itching, swelling, tissue prolapse, pain, bowel habits, and how long the issue has been going on. This is followed by an exam to determine whether the source is internal hemorrhoids, external hemorrhoids, an anal fissure, or another anorectal condition.
That distinction is important because bright red bleeding with bowel movements may be hemorrhoids, but severe tearing pain is often more consistent with a fissure. Treatment works best when the diagnosis is specific.
If you are a candidate for an office procedure, treatment may happen the same day or be scheduled soon after, depending on the findings. Many patients are surprised by how brief and structured the process is. There is no hospital check-in, no general anesthesia, and usually no need to put your life on hold.
Recovery after office based hemorrhoid treatment
Recovery is one of the biggest reasons patients pursue this route. Most people can return to normal daily activity quickly, often the same day, with some simple instructions around bowel habits, hydration, and avoiding strain.
That does not mean zero recovery. Some patients feel temporary pressure, mild discomfort, or fullness after banding. Others may need a short period of medication use and supportive care. The key difference is scale. Recovery is generally far lighter than what patients expect from traditional hemorrhoid surgery.
It also helps to be realistic. If constipation, straining, prolonged sitting on the toilet, or low fiber intake continue, symptoms can come back. Treatment addresses the current problem, but bowel habits still matter for long-term control.
Who is a good candidate for office based hemorrhoid treatment
Patients with internal hemorrhoids that bleed, prolapse, itch, or create recurring irritation are often good candidates. It is especially appealing for people who want to avoid anesthesia, limit downtime, and get treated by a provider who focuses on this condition.
It may also be a good fit if over-the-counter care has stopped working. Many adults spend months rotating between creams, suppositories, and home remedies without lasting improvement. Once symptoms become recurrent or disruptive, a procedure-based solution often makes more sense than repeating the same temporary measures.
The best candidates are not defined only by symptom severity. They are also people who want clarity. If you are not sure whether you have hemorrhoids, a fissure, or something else, a specialist evaluation can answer that quickly and point you toward the most effective next step.
Why specialization makes a difference
Hemorrhoids are common, but treatment quality still varies. In a general setting, anorectal symptoms may be one small part of a much broader practice. In a specialty model, the focus is narrower and the workflow is built around fast diagnosis and minimally invasive treatment.
That tends to matter in three ways. First, specialized providers are more likely to distinguish between similar symptoms that need different treatment. Second, office processes are designed for efficiency and privacy. Third, patients often feel more comfortable when they know they are seeing a team that treats these conditions every day.
At Hemorrhoid Centers of America, that focused model is built around non-surgical relief, office-based procedures, and helping patients return to regular life without the delays and recovery burdens that often keep people from seeking care.
When not to keep waiting
A small amount of irritation after constipation is one thing. Ongoing bleeding, repeated swelling, prolapse, worsening discomfort, or symptoms that keep returning are another. If hemorrhoids are interfering with your job, workouts, travel, or confidence, the problem is already worth evaluating.
The same is true if pain is significant or your symptoms do not match what you expected from hemorrhoids. A proper exam can confirm the diagnosis and rule out other causes of rectal pain or bleeding. That is not overreacting. It is how you avoid spending more time and money on treatments that were never likely to work.
Relief does not always require surgery, and it does not have to take over your schedule. For many patients, the most effective next step is also the most practical one: getting the problem evaluated in a setting built to treat it quickly, discreetly, and well.