Same Day Hemorrhoid Treatment Options
March 22, 2026
How to Stop Hemorrhoid Bleeding Safely
March 26, 2026If you are weighing hemorrhoid banding vs surgery, you are probably past the point of hoping creams, wipes, and home remedies will fix the problem. Many patients reach this stage after weeks or months of bleeding, itching, swelling, or pain, and the question is usually not whether to get treated. It is which treatment will actually solve the problem with the least disruption to your life.
That is the right question to ask. Banding and surgery are not interchangeable, and the best option depends on the type of hemorrhoid, the severity of symptoms, and how much recovery time you can realistically take on.
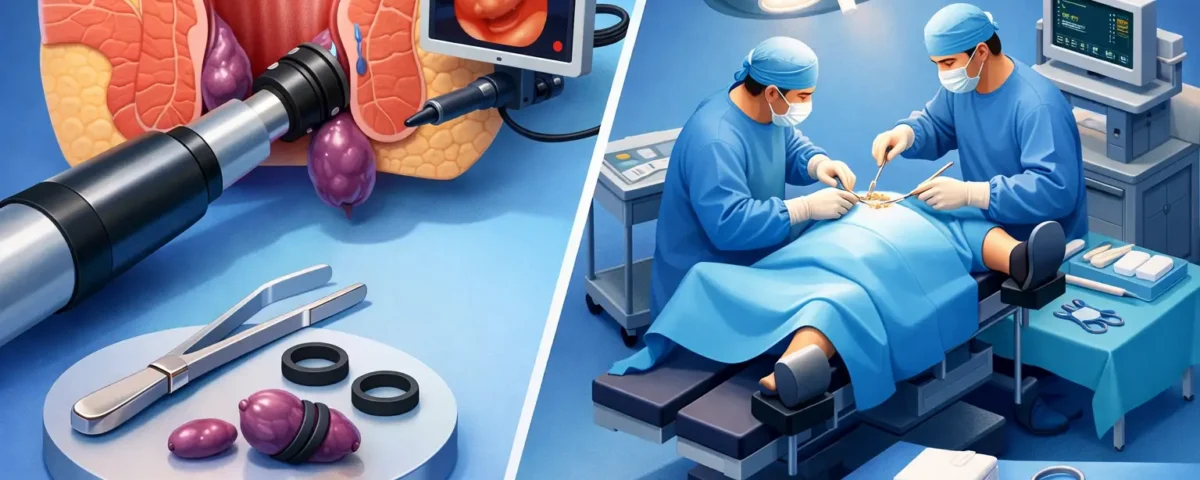
Hemorrhoid banding vs surgery: the core difference
Hemorrhoid banding is a non-surgical, office-based procedure most often used for internal hemorrhoids. A provider places a small band around the base of the hemorrhoid, cutting off its blood supply. The treated tissue shrinks and falls away over time. There is no traditional incision, no hospital stay, and no general anesthesia.
Surgery is a broader category. It usually refers to hemorrhoidectomy, which removes hemorrhoidal tissue, or in some cases stapled procedures used for more advanced internal hemorrhoids. Surgery is generally reserved for cases that are more severe, more complicated, or less likely to respond to office-based treatment.
For most patients, the practical difference comes down to invasiveness, downtime, and recovery. Banding is designed to treat the problem efficiently while letting you return to normal activity quickly. Surgery can be highly effective, but it is a more involved path.
When banding is often the better fit
Banding is commonly a strong option for symptomatic internal hemorrhoids, especially when bleeding, prolapse, pressure, or irritation keeps coming back. It is often appealing to patients who want relief without anesthesia, stitches, or a prolonged recovery.
This matters because many adults delay care for one simple reason: they do not want surgery. They worry about pain, missed work, or the idea of a hospital-based procedure for a very personal problem. Office-based banding addresses that concern directly. In many cases, treatment is fast, discreet, and compatible with a normal schedule.
Another advantage is that banding targets the source of the symptoms rather than simply masking them. Over-the-counter products may temporarily ease irritation, but they do not remove the internal hemorrhoid tissue causing repeated bleeding or prolapse. Banding is often the step between ineffective self-care and full surgical intervention.
That said, banding is not for every hemorrhoid. It is typically used for internal hemorrhoids, not external hemorrhoids, thrombosed external hemorrhoids, or every advanced mixed case.
When surgery may be necessary
Surgery still has an important role. Some hemorrhoids are too large, too advanced, or too complex for banding alone. If a patient has substantial external hemorrhoids, significant prolapse, recurrent symptoms after multiple treatments, or anatomy that is not a good fit for office procedures, surgery may be the better choice.
This is where honest evaluation matters. A specialized provider should not push every patient into one pathway. The goal is not to avoid surgery at all costs. The goal is to avoid unnecessary surgery while recognizing when it is truly the most effective option.
For a smaller subset of patients, surgery provides a more definitive answer because it removes tissue directly. The trade-off is that the recovery is usually more intense.
Pain and discomfort: what patients usually care about most
When patients compare hemorrhoid banding vs surgery, pain is usually at the top of the list. Understandably so.
Banding is generally associated with less disruption than surgery. Because internal hemorrhoids originate in an area with fewer pain-sensitive nerves, many patients describe banding as pressure or fullness rather than sharp pain. Some soreness, cramping, or the urge to have a bowel movement can happen after treatment, but the experience is usually manageable.
Surgery is different. Hemorrhoidectomy can involve significant postoperative pain because it treats tissue in a more sensitive area and requires a longer healing period. Pain control is part of the treatment plan, but recovery is still a bigger event. For patients with demanding jobs, caregiving responsibilities, or limited ability to take time off, that can be a major factor.
Pain is never the only consideration, but it is a practical one. If two treatments could work, the one with less discomfort and less downtime often makes more sense.
Recovery time and return to normal life
This is where the difference becomes very real.
With banding, many patients return to regular daily activities the same day or shortly after treatment. They may need to avoid heavy straining for a short period, but they are typically not facing a long interruption to work or routine. That convenience is not a minor benefit. For a lot of people, it is the reason they finally move forward with treatment.
With surgery, recovery is more involved. Depending on the procedure and the individual patient, healing can take weeks. Bowel movements may be painful during recovery, activity may be limited, and follow-up care tends to be more intensive.
Neither option should be judged on convenience alone. Still, when banding is clinically appropriate, the shorter recovery is one of its clearest advantages.
Effectiveness depends on choosing the right patient
Banding can be highly effective for the right type of hemorrhoid. That phrase matters: for the right type of hemorrhoid.
A lot of frustration in hemorrhoid care comes from mismatched treatment. Patients either spend too long trying home remedies for a condition that needs a procedure, or they assume surgery is the only serious option when a non-surgical treatment could work well.
A focused anorectal evaluation helps sort that out. Internal hemorrhoids, external hemorrhoids, anal fissures, skin tags, and other causes of rectal symptoms can overlap. Bleeding does not always mean the same thing. Pain does not always point to the same diagnosis. The treatment decision should come after an exam, not before one.
At a specialized center, that evaluation is geared toward finding the least invasive treatment that can still solve the problem effectively. That is a meaningful distinction from a more general setting where surgery may be presented earlier in the process.
Who should think carefully before choosing surgery first
If your main symptoms are internal bleeding, irritation, or prolapsing hemorrhoids and you have not yet had a specialized exam, it may be too early to assume surgery is necessary. The same is true if your biggest concern is avoiding anesthesia or missing work.
Patients in these situations often benefit from hearing whether office-based treatment is still on the table. Hemorrhoid Centers of America is built around that question, with board-certified surgeons focused on non-surgical treatment pathways when they are clinically appropriate.
That does not mean banding wins every comparison. It means surgery should be chosen because it is necessary, not because it is the only option a patient happened to hear about.
Questions worth asking at your appointment
A good consultation should make the decision clearer, not more confusing. Ask what type of hemorrhoid you have, whether it is internal or external, whether banding is a candidate option, and what recovery will realistically look like with each treatment.
You should also ask about the likely number of treatments, the expected timeline for symptom relief, and whether your symptoms could be caused by something else such as an anal fissure. These questions help you compare not just procedures, but outcomes.
The better choice is the one that matches the problem
For many patients, hemorrhoid banding offers the balance they want most: effective treatment, no traditional surgery, minimal downtime, and a fast return to normal life. For others, surgery is still the right call because the hemorrhoids are too advanced or too complex for office treatment alone.
The key is not choosing the most aggressive option. It is choosing the option that fits your actual condition and your life. If you have been putting this off because you assumed treatment had to mean surgery, it may be worth finding out whether a simpler path can get you real relief.