How to Stop Hemorrhoid Bleeding Safely
March 26, 2026
Best Non Surgical Hemorrhoid Treatments
March 30, 2026If you are dealing with bleeding, itching, pressure, or swelling from internal hemorrhoids, you probably want one clear answer: how office hemorrhoid banding works, and whether it can help without surgery. That is a reasonable question, especially if creams, wipes, and home remedies have not solved the problem or the symptoms keep coming back.
Office hemorrhoid banding is a non-surgical treatment used for internal hemorrhoids. The goal is simple. A physician places a very small band around the base of the hemorrhoid inside the rectum, which cuts off its blood supply. Over time, the treated tissue shrinks, separates, and passes naturally, allowing the area to heal.
For many patients, the appeal is not just that it works. It is that it is done in the office, does not usually require anesthesia, and often allows you to get back to normal activity the same day.
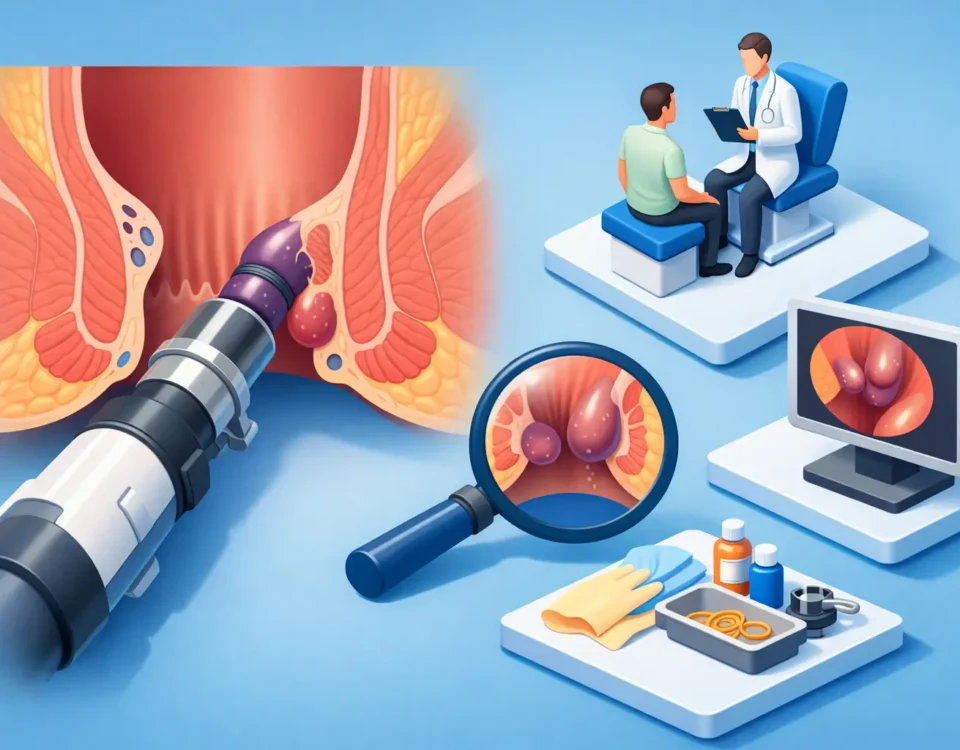
How office hemorrhoid banding works in simple terms
Internal hemorrhoids are enlarged veins and supporting tissue inside the rectum. When they become irritated or prolapse, they can cause bright red bleeding, mucus, itching, pressure, and a feeling that something is not quite right during or after a bowel movement.
Banding treats the problem at its source. During the procedure, the physician uses a specialized instrument to position a tiny rubber band around the hemorrhoid tissue above the sensitive pain line. That location matters. Internal hemorrhoids usually have fewer pain-sensitive nerves than external hemorrhoids, which is one reason banding can often be done comfortably in an office setting.
Once the band is in place, blood flow to that hemorrhoid is reduced. Without that blood supply, the tissue gradually shrinks. In the days that follow, the banded tissue separates and passes on its own, usually without the patient noticing exactly when it happens. A small scar forms as the area heals, which can help support the tissue and reduce future prolapse.
That is the basic mechanics of how office hemorrhoid banding works. It is targeted, local treatment designed to stop ongoing symptoms without the recovery demands of traditional hemorrhoid surgery.
What happens during the appointment
Most patients are surprised by how straightforward the visit is. The first step is confirming that hemorrhoids are actually the cause of your symptoms. Not every case of rectal bleeding, irritation, or pain is caused by hemorrhoids, so an exam matters. A specialist may use a small scope to evaluate the anal canal and lower rectum, identify internal hemorrhoids, and determine whether banding is appropriate.
If you are a candidate, the procedure itself is usually brief. You are positioned for the exam, and the physician uses an office-based banding device to place one or more bands on the internal hemorrhoid tissue. The exact number depends on the severity and location of the hemorrhoids. In some cases, treatment is staged over more than one visit to improve comfort and healing.
Most patients describe the sensation as pressure, fullness, or an urge to have a bowel movement rather than sharp pain. That said, comfort can vary. If a band is placed too low or an individual is especially sensitive, the area can feel more uncomfortable. When the procedure is performed by an experienced provider focused on hemorrhoid treatment, placement is more precise, which matters both for results and for comfort.
Afterward, you can usually leave the office on your own and return to the rest of your day with minimal disruption.
What the procedure feels like afterward
The first 24 to 48 hours are often the period when patients notice the most pressure or awareness in the area. Some people feel almost nothing. Others describe a dull ache, a sensation of fullness, or mild cramping. This is generally manageable and short-lived.
You may also notice a small amount of bleeding several days later, often around the time the treated tissue separates. Light bleeding can be expected, but heavy bleeding is not. Your physician should give you clear instructions about what is normal, what to avoid, and when to call.
One important detail is that office banding is designed for internal hemorrhoids. If someone has significant external hemorrhoids, a painful thrombosed hemorrhoid, or another anorectal condition, banding may not be the best fit. That is why a proper diagnosis comes first.
When banding is a good option
Banding is commonly used for symptomatic internal hemorrhoids, especially when bleeding and prolapse are recurring problems. It is often recommended for patients who have already tried increasing fiber, drinking more water, using stool softeners, or relying on over-the-counter products without enough relief.
It can be an especially good fit for people who want definitive treatment but want to avoid anesthesia, hospital-based procedures, or a long recovery. That includes busy professionals, parents, caregivers, and older adults who do not want their schedule turned upside down by treatment.
Still, it depends on the severity of the hemorrhoids and the full picture of your symptoms. A patient with mild internal hemorrhoids may improve with conservative care alone. A patient with more advanced disease, mixed internal and external hemorrhoids, or another condition such as an anal fissure may need a different treatment plan.
How quickly symptoms improve
Banding does not always create instant relief the same day, because the treated tissue needs time to shrink and heal. Some patients notice improvement in bleeding fairly quickly. For others, the change is more gradual over days to weeks.
The timeline also depends on which symptom is bothering you most. Bleeding often improves earlier than tissue prolapse. Itching and irritation may improve as swelling and mucus decrease. If constipation or straining continues after treatment, symptoms can linger or recur, which is why aftercare and bowel habits are part of the overall plan.
Many patients need more than one banding session to fully address multiple hemorrhoids. That does not mean the treatment is failing. It simply reflects the fact that hemorrhoids can occur in different columns of tissue, and treating them in stages is often the safest and most comfortable approach.
Recovery and downtime
One of the biggest reasons patients ask about office banding is recovery. In most cases, downtime is minimal. Many people return to work, drive themselves home, and resume regular non-strenuous activity the same day.
That does not mean you should ignore aftercare. You may be advised to avoid heavy lifting for a short period, stay well hydrated, increase fiber, and keep bowel movements soft to reduce strain on the healing tissue. Those steps are not minor. They support healing and help lower the chance of irritation or recurrence.
You should also follow medication instructions carefully, especially if you take blood thinners or medications that affect bleeding risk. Your physician will advise you on what is safe based on your medical history.
Benefits and trade-offs to understand
The main benefits are clear. Office hemorrhoid banding is minimally invasive, usually fast, does not typically require anesthesia, and avoids the recovery associated with surgical hemorrhoidectomy. For many internal hemorrhoids, it is an effective way to control bleeding, shrink prolapsing tissue, and help patients move on from a cycle of temporary symptom management.
The trade-off is that it is not a one-size-fits-all treatment. Some patients need multiple visits. Some have anatomy or symptoms that make another option more appropriate. And while banding is highly effective for the right problem, no procedure can fully overcome ongoing straining, chronic constipation, or other habits that continue to put pressure on the area.
That is why specialized evaluation matters. A provider who treats hemorrhoids every day is more likely to distinguish between symptoms that are banding-related, fissure-related, external disease, or something else entirely.
Why specialized care makes a difference
Hemorrhoid treatment is often delayed because patients feel embarrassed or assume they just need to live with the symptoms. But persistent bleeding, swelling, or irritation deserves a real evaluation. The right office-based procedure can be much simpler than people expect.
At a focused specialty practice such as Hemorrhoid Centers of America, the process is built around prompt diagnosis, non-surgical treatment, and getting patients back to normal life quickly. That focus matters when you want clear answers, efficient care, and a treatment plan designed around relief rather than a default path to surgery.
Questions patients often have before scheduling
A common concern is whether the procedure is painful. For most patients, it is more uncomfortable than painful, with pressure being the most common sensation. Another concern is whether the hemorrhoid comes back. The treated hemorrhoid tissue can be effectively addressed, but new or recurrent hemorrhoid symptoms can still happen over time, especially if bowel habits continue to strain the area.
Patients also ask whether bleeding always means hemorrhoids. The answer is no. Hemorrhoids are common, but rectal bleeding should be properly evaluated instead of self-diagnosed. That is one of the strongest reasons not to rely only on home treatment when symptoms persist.
If your symptoms are interfering with work, exercise, travel, or simply sitting comfortably through the day, waiting usually does not make the issue easier to manage. Getting it checked does not commit you to surgery. In many cases, it opens the door to a simpler solution that can be handled in the office with much less disruption than you expected.
You do not need to keep arranging your day around discomfort, bleeding, or worry about the next flare-up. When the diagnosis is clear and the treatment is matched to the problem, relief can be much closer than most patients think.