How to Shrink Prolapsing Hemorrhoids
May 13, 2026
Hemorrhoid Symptoms vs Anal Fissure
May 17, 2026A prolapsed hemorrhoid can turn an ordinary day into a constant distraction. Sitting at work, using the bathroom, walking, and even trying to sleep can become uncomfortable fast. This guide to prolapsed hemorrhoid care explains what is happening, what you can do right away, and when it makes sense to seek prompt medical treatment instead of continuing to wait it out.
What a prolapsed hemorrhoid actually means
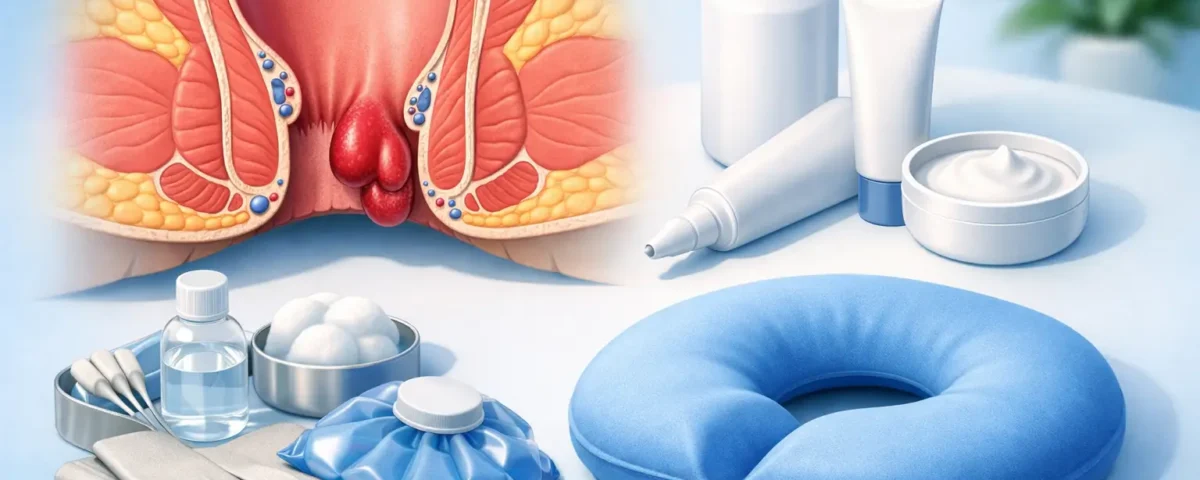
Hemorrhoids are swollen veins in the lower rectum or anus. When an internal hemorrhoid pushes down and bulges outside the anal opening, it is called a prolapsed hemorrhoid. Some prolapsed hemorrhoids go back inside on their own. Some need to be gently pushed back in. Others stay outside and continue to cause pain, irritation, swelling, mucus, or bleeding.
That difference matters because treatment depends on how severe the prolapse is and how often it happens. Mild symptoms may improve with conservative care. Recurrent prolapse, persistent bleeding, or tissue that stays outside usually points to a problem that home remedies alone may not fully resolve.
Guide to prolapsed hemorrhoid care at home
If symptoms are recent and manageable, home care can reduce irritation and help calm a flare-up. The goal is simple – decrease pressure, reduce inflammation, and avoid further straining.
Start with bowel habits. Hard stools and repeated straining are two of the biggest reasons hemorrhoid symptoms continue. Increasing fiber through food or a fiber supplement can help stools pass more easily. Drinking more water often helps fiber work better. If constipation is part of the problem, a stool softener may be useful for a short period, especially during an active flare.
Warm sitz baths can also help. Sitting in a few inches of warm water for 10 to 15 minutes may ease sphincter spasm, reduce irritation, and make the area feel less raw. This will not remove the hemorrhoid itself, but it can make the symptoms easier to tolerate.
Over-the-counter products may provide temporary relief. Creams, wipes, and suppositories can sometimes reduce itching or burning, though they do not treat the underlying enlarged hemorrhoid. Some products can also irritate sensitive skin if used too often or for too long. If a product seems to make the area sting more, stop using it.
Cold compresses can help with swelling, especially if the prolapsed tissue feels inflamed after a bowel movement. Gentle hygiene matters too. Harsh wiping tends to make symptoms worse. Cleaning the area with water or soft, unscented tissue is usually more comfortable.
If the hemorrhoid prolapses during a bowel movement and is not severely painful, some patients can gently push it back inside with a clean, lubricated finger. This should never be forced. If the tissue is very painful, dark, or difficult to reduce, it is better to stop and get evaluated.
What not to do during a flare
Many people make symptoms worse without realizing it. Sitting on the toilet for long stretches, scrolling on the phone, straining to finish a bowel movement, or repeatedly checking the area can all increase pressure and swelling.
Heavy lifting may also aggravate prolapse, especially during an active flare. That does not mean complete bed rest is necessary. Light walking is often better than sitting all day. The goal is to avoid the specific activities that sharply increase abdominal and rectal pressure.
It is also worth being careful with self-diagnosis. Not every lump, bleed, or painful bowel movement is caused by hemorrhoids. Anal fissures, skin tags, abscesses, and other conditions can look or feel similar.
Cuando la atención domiciliaria no es suficiente
Home care is reasonable for mild, short-lived symptoms. It becomes less reasonable when the same problem keeps returning or starts interfering with your routine. If you are planning your day around pain, carrying creams everywhere, or worrying about every bowel movement, that is usually a sign the problem deserves more than temporary symptom control.
Bleeding is another reason to stop guessing. Bright red blood with hemorrhoids is common, but ongoing rectal bleeding should still be evaluated. The same is true for tissue that remains prolapsed, increasing pain, drainage, or symptoms that do not improve after a week or two of conservative care.
Severe pain can suggest a thrombosed external hemorrhoid or a prolapsed internal hemorrhoid with significant swelling. If the tissue looks dark purple or black, or the pain feels sudden and intense, prompt medical assessment is important.
How specialists evaluate prolapsed hemorrhoids
A focused exam can usually clarify what type of hemorrhoid is present and how advanced it is. That is one advantage of seeing a provider who treats hemorrhoids every day rather than folding anorectal symptoms into a broader surgical practice.
The visit is typically more straightforward than patients expect. A specialist will review symptoms such as bleeding, itching, swelling, prolapse, bowel habits, and prior treatments. Then they examine the area to determine whether the issue is internal hemorrhoids, external hemorrhoids, fissures, or another condition. That distinction matters because the right treatment for one condition may do very little for another.
For patients who have delayed care out of embarrassment, this is often the turning point. Once the diagnosis is clear, treatment decisions become more practical and less stressful.
Office-based treatment for prolapsed hemorrhoids
For many internal prolapsed hemorrhoids, office-based treatment can provide more definitive relief than ongoing cycles of creams and waiting. One of the most common non-surgical options is hemorrhoid banding. In the right patient, banding targets the internal hemorrhoid at its source, cutting off blood flow so the tissue shrinks and resolves over time.
This approach is especially appealing for patients who want to avoid traditional surgery, anesthesia, and extended downtime. It is not the right fit for every hemorrhoid. External hemorrhoids, mixed hemorrhoids, clotting, fissures, and the degree of prolapse all influence the plan. But for properly selected internal hemorrhoids, office treatment can be efficient and highly effective.
That is where specialized care matters. A center focused on non-surgical hemorrhoid treatment can match the procedure to the anatomy and symptom pattern rather than moving too quickly toward hospital-based surgery. At Hemorrhoid Centers of America, that focus is central to care.
What recovery usually looks like
Recovery depends on the treatment used and how inflamed the hemorrhoid is before treatment. With conservative care alone, symptoms may improve gradually, but flare-ups often return if the underlying issue remains. With office-based treatment, many patients resume normal activity quickly, though mild pressure or temporary irritation can occur.
The best recoveries usually involve more than the procedure itself. Patients still need to address constipation, low-fiber eating patterns, dehydration, and habitual straining. Otherwise, new hemorrhoids can develop or residual symptoms can linger.
This is also where expectations matter. If a hemorrhoid has been prolapsing for months, treatment may not feel like flipping a switch overnight. Relief is often significant, but the timeline varies with severity and the exact treatment plan.
Cuándo es mejor acudir al médico cuanto antes
You do not need to wait until symptoms are unbearable. If prolapse is recurring, if bleeding keeps happening, or if home remedies are only buying short periods of relief, it is reasonable to schedule an evaluation. The same goes for patients who are avoiding travel, exercise, intimacy, or work comfort because of hemorrhoid symptoms.
Earlier treatment can sometimes mean a simpler treatment path. Waiting through repeated flare-ups often means more swelling, more irritation, and more frustration. For many patients, the real relief comes from finally getting a clear diagnosis and a treatment plan that fits real life.
A prolapsed hemorrhoid is common, but it should not be dismissed as something you simply have to manage forever. The right care can reduce pain, bleeding, and disruption without pushing you straight into surgery, and that can make everyday life feel normal again.